novel techniques to cure a difficult problem
personalized care.
robotic precision.
While a rare diagnosis, superior mesenteric artery syndrome has not had a near 100% durable treatment. Until now. Robotic anterior duodenal transposition is a new technique developed by Dr. Le for this disease, which has a near 100% cure rate, so you can get back to living life.
Summary
For details, continue scrolling
▾
-
Superior mesenteric artery syndrome is a rare cause of duodenal obstruction, whose only possibility of treatment is surgery.
-
Because the ultimate end result of this disease is bowel obstruction in the upper abdomen, symptoms include early fullness after even a small meal, nausea, bloating, vomiting, and eventual food fear that can lead to weight loss and malnutrition.
-
Testing involves imaging, such as CT scan or upper GI x-ray, as well as upper endoscopy performed by a trained specialist such as a gastroenterologist.
-
Surgery is the only truly curative treatment. Most commonly, this is done with a type of bowel bypass, which can have side effects. Dr. Le has developed a new technique that maintains normal bowel function and pathways, minimizing or even eliminating side effects.
Superior Mesenteric
Artery Syndrome (SMAS)
Superior Mesenteric Artery (SMA) Syndrome is a rare condition where the third portion of the duodenum becomes compressed between the aorta and the superior mesenteric artery, creating a partial or complete blockage. This occurs when the angle between these two vessels becomes abnormally narrow, often due to rapid weight loss, anatomical variation, or conditions affecting fat pad thickness around the SMA. The resulting compression can lead to gastric outlet obstruction, impairing normal digestion and causing significant nutritional challenges.
Diagnosis typically involves imaging studies such as CT angiography or an upper GI series, confirming the narrowing and delayed gastric emptying.
Symptoms of Superior Mesenteric Artery (SMA) Syndrome result from compression of the duodenum, leading to partial or complete gastric outlet obstruction. Patients often experience persistent nausea, vomiting (especially of undigested food or bile), abdominal pain, bloating, and early satiety (feeling full quickly). Symptoms are typically worse after eating and may improve when lying in a knees-to-chest position, which can temporarily relieve the compression. Due to chronic difficulty with eating, significant weight loss and malnutrition are common, further exacerbating the problem by reducing the fat pad that cushions the SMA. Without proper diagnosis and treatment, SMA Syndrome can lead to severe dehydration, electrolyte imbalances, and long-term nutritional deficiencies, requiring urgent medical or surgical intervention.
Superior Mesenteric artery syndrome: A systematic review - Scientific Figure on ResearchGate. [accessed 10 Feb, 2025] ResearchGate
Treatment for Superior Mesenteric Artery (SMA) Syndrome focuses on restoring nutrition, relieving duodenal compression, and improving symptoms. In mild to moderate cases, the primary approach is aggressive nutritional support, including high-calorie diets, enteral (tube) feeding, or total parenteral nutrition (TPN) if oral intake is insufficient. Weight gain can help increase the fat pad between the SMA and aorta, widening the angle and relieving compression.
However, in severe or persistent cases, or when conservative measures fail, surgical intervention may be required. Procedures such as duodenojejunostomy (bypassing the compressed section of the duodenum) or Strong’s procedure (repositioning the duodenum) offer long-term relief. The anatomic alteration of this procedure can potentially to significant side effects, such as sump syndrome, obstruction, and the need for possible future revisional surgeries to address these side effects.
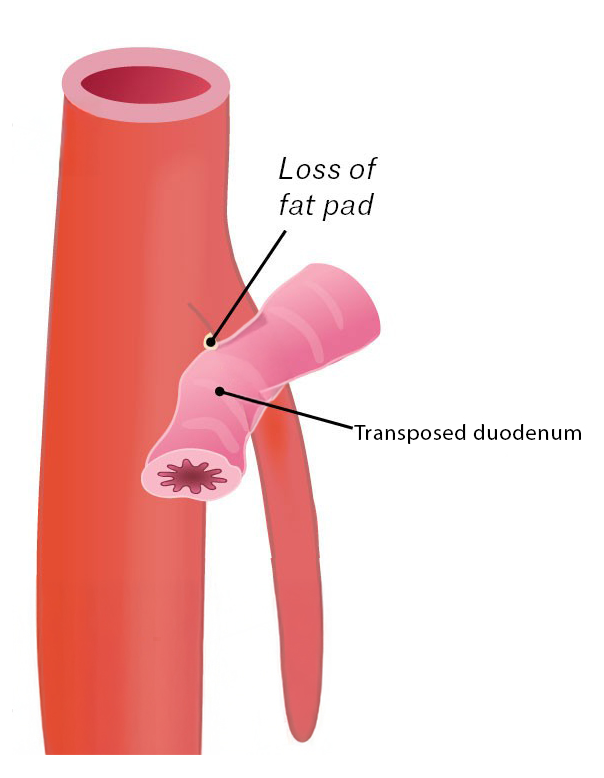
A new surgical approach for Superior Mesenteric Artery (SMA) Syndrome, called robotic anterior duodenal transposition, offers an innovative, minimally invasive solution that preserves the natural flow of digestion while ensuring a quicker recovery. Unlike traditional bypass procedures, this technique involves mobilizing and repositioning the third portion of the duodenum anterior to the SMA, effectively eliminating the compression without rerouting the digestive tract. Robotic technology enhances precision, allowing for meticulous dissection, reduced tissue trauma, and improved nerve preservation. This approach maintains a more physiologic path for food transit, reducing the risk of complications like bacterial overgrowth or malabsorption seen in bypass procedures. With smaller incisions, less postoperative pain, and a faster return to normal eating, robotic anterior duodenal transposition is emerging as a preferred surgical option for patients with severe SMA Syndrome who require definitive treatment.
Robotic sma syndrome surgery
Due to Dr. Le’s innovative approaches to rare surgical diseases, a new type of surgery has been developed robotically where the compressed portion of the duodenum is transposed above the SMA, to keep the pathway and flow of food physiologically normal, without alteration of normal anatomy. The magnified view and extreme precision of robotic surgery allows for the most natural repair of this rare but significant disease, speeding your recovery process.
Before Surgery
You will be seen by Dr. Le in the clinic for a comprehensive history and physical, and to discuss your symptoms specific to your problem.
Testing for SMA Syndrome usually involves CT scan, upper endoscopy, and upper GI follow-through x-rays.
Follow up visit or telehealth visit to discuss results of testing if needed.
Smoking cessation for 2 weeks before and 2 weeks after surgery to lower anesthetic risks.
Prepare for surgery.
After Surgery
Most of the time, you will be admitted overnight for monitoring.
No heavy lifting more then 30 lbs for 2-3 weeks, with a slow and steady increase back to normal activity over 2 weeks after that.
You will be permitted to shower 24 hours after your surgery, patting dry the areas of your incisions.
A soft mushy diet, free from meat, chewy breads, and carbonated beverages for 1-2 weeks after surgery will be recommended.
You will be scheduled for at least one followup visit about 1 week after your operation.
additional services we offer
STOMACH PROBLEMS
Trusted expertise in a vast range of surgical and functional stomach problems that can often present with vague symptoms, finally getting you answers.
HERNIAS
Innovative approaches to all types of abdominal and groin hernias, decreasing pain and allowing faster return to everyday activities.
SMALL BOWEL DISEASES
Leading-edge surgical techniques in a wide array of common and uncommon small bowel diseases, supporting you in your treatment journey.
REFLUX & HEARTBURN
Tailored surgical treatments specific to each patient, with the ultimate goal of eliminating heartburn and getting you off of your acid-blocking medications.
COLON DISEASES
Progressive, patient-centered operations and treatments, from hemorrhoids to colon cancer, decreasing your time in the hospital so you can get home faster.
GENERAL SURGERY
Lumps and bumps, lacerations, cysts, and many other problems can be treated by general surgeons.
MALS
Median arcuate ligament syndrome, a rare and difficult diagnosis, requires expertise and precision to treat. See why Dr. Le is at the forefront.
GALLBLADDER DISEASES
Cutting edge techniques to remove the gallbladder through “hidden incisions,” as well as single-anesthesia operations to remove stones stuck in the biliary tubes.